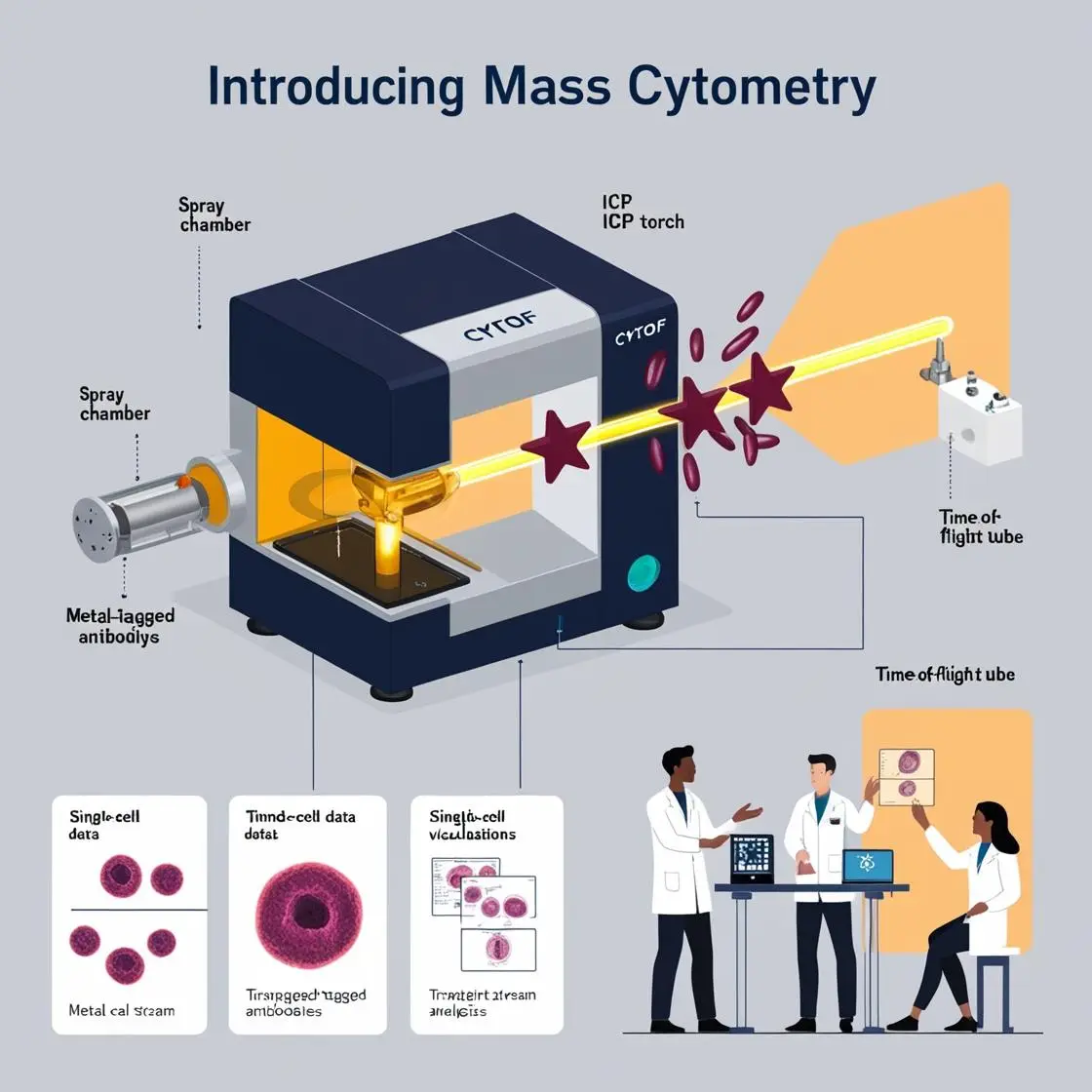
Allergies and hypersensitivity reactions are increasingly prevalent, affecting millions worldwide and significantly impacting daily life. Mass cytometry has emerged as a powerful tool for unraveling the complex immune responses underlying these conditions, offering new insights that translate into practical benefits for patients.
Profiling Allergen-Specific Immune Responses
Mass cytometry has revolutionized our ability to characterize allergen-specific immune responses with unprecedented detail. The groundbreaking study by Chiang et al. (2018) in the Journal of Allergy and Clinical Immunology used single-cell RNA sequencing and flow cytometry to profile peanut-responsive T cells in patients with peanut allergy. They uncovered heterogeneous effector TH2 subsets, revealing a complexity in allergic responses previously unappreciated.
This detailed understanding could lead to more precise diagnostic tests. For instance, a child suspected of having a peanut allergy might undergo a blood test analyzed by mass cytometry, potentially avoiding the need for risky oral food challenges. The test could not only confirm the allergy but also provide information about its severity, allowing for more tailored management strategies.
Mechanisms of IgE-Mediated Hypersensitivity
Mass cytometry has shed new light on the intricate mechanisms of IgE-mediated hypersensitivity, the primary driver of allergic reactions. A pivotal study by Neeland et al. (2020) published in Nature Copmmunications, “Mass cytometry reveals cellular fingerprint associated with IgE+ peanut tolerance and allergy in early life,” utilized high-dimensional mass cytometry to identify distinct immune signatures associated with peanut allergy (PA) and peanut-sensitized tolerance (PST) in infants. Key findings include increased activated B cells and TNFα production in PA, while PST was characterized by reduced naive CD4 T cells and increased plasmacytoid dendritic cells.
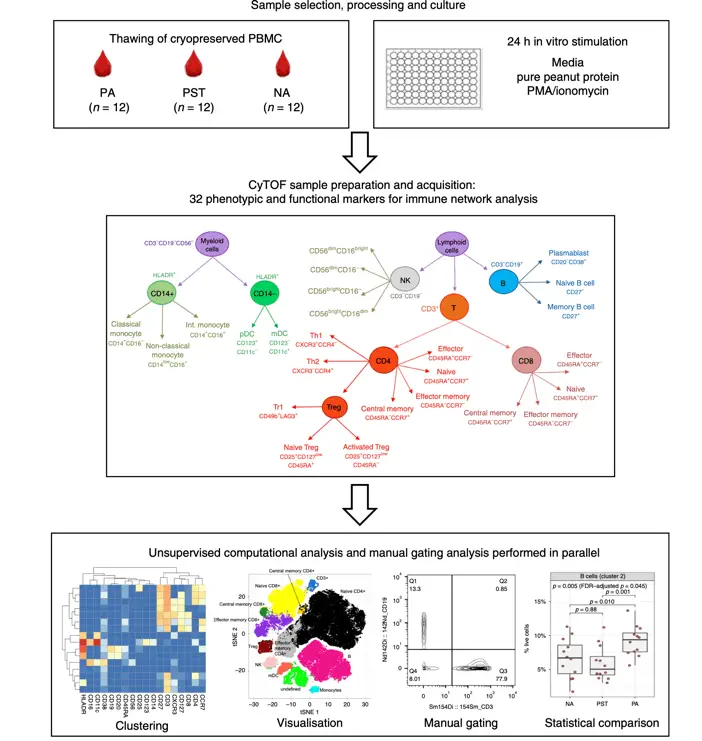
Monitoring Desensitization Therapies
Mass cytometry has proven invaluable in monitoring and optimizing desensitization therapies, offering hope to many allergy sufferers. A study by Wambre et al. (2017) in Journal of Allergy and Clinical Immunology, cited over 350 times, “A phenotypically and functionally distinct human TH2 cell subpopulation is associated with allergic disorders,” used mass cytometry to identify a specific subset of TH2 cells associated with allergies. More importantly, they showed that successful allergen immunotherapy was associated with the deletion of these pathogenic TH2 cells.
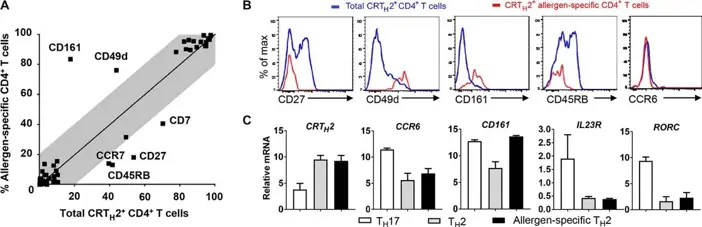
This research could transform how allergen immunotherapy is monitored and personalized. A patient undergoing desensitization for grass pollen allergy, for instance, might have their blood analyzed periodically using mass cytometry. The gradual disappearance of these pathogenic TH2 cells could indicate that the therapy is working, even before the patient experiences symptomatic improvement. This could allow for real-time adjustments to the treatment regimen, optimizing its effectiveness.
Real-World Impact
The insights gained from mass cytometry studies are translating into tangible benefits for allergy sufferers:
- Personalized Treatment Plans: By profiling an individual’s allergen-specific immune response, doctors can tailor treatments more effectively. A patient whose mass cytometry profile shows a predominance of certain T cell subsets might be recommended for a specific type of immunotherapy or medication.
- Improved Diagnostics: Mass cytometry could lead to more accurate allergy tests, reducing false positives and negatives. This could prevent unnecessary dietary restrictions or missed diagnoses, significantly improving quality of life for many individuals.
- Novel Therapeutic Targets: The detailed cellular profiles revealed by mass cytometry are identifying new targets for drug development. Future allergy medications might target specific cell subsets or signaling pathways identified through this technology, potentially offering more effective and less side-effect-prone treatments.
- Early Intervention: By identifying markers of allergic predisposition before symptoms manifest, mass cytometry could enable preventive strategies. For instance, infants at high risk of developing food allergies might be identified early and enrolled in proactive desensitization programs.
As mass cytometry technology continues to advance, we can anticipate even more precise and personalized approaches to allergy management. From the child with a life-threatening peanut allergy to the adult struggling with chronic hives, the insights gained from this technology are paving the way for a future where allergies no longer dictate lifestyles or threaten lives.
The symphony of cellular interactions underlying allergic responses, once a cacophony of misunderstood reactions, is gradually being deciphered through the high-resolution lens of mass cytometry. Each new discovery brings us closer to conducting this immune orchestra in harmony, transforming the discordant notes of hypersensitivity into a more manageable melody of immune function. As we continue to unravel these complex cellular interactions, we move steadily towards a world where allergies are not just managed, but potentially prevented or cured, liberating millions from the burden of hypersensitivity and allowing them to embrace life without fear of allergic reactions.
From the lab bench to the factory floor, my journey through immunology has been quite the ride. At Novartis Huningue, I found myself elbow-deep in the production of Xolair, an anti-IgE monoclonal antibody that's a lifesaver for allergy sufferers. It was like watching the circle of life, but for antibodies - from discovery to large-scale production, all under one roof. But the real fun? That was back in the lab, brewing up our very own PDL1 antibodies. Let me tell you, producing antibodies is less like haute cuisine and more like milking a very, very tiny cow. There I was, coaxing these microscopic factories to churn out our cellular gold. It was oddly satisfying, like being a farmer for science. From pipetting microliters to overseeing hectoliters, I've seen antibodies in all their glory. It's a strange world where the same principles apply whether you're making a thimbleful or a swimming pool's worth of antibodies.
Guillaume Beyrend